Assessment of dental implant surface stability at the nanoscale level
Link: https://www.sciencedirect.com/science/article/pii/S0109564122000689#fig0065
Varvara Labisa Ernest Bazikyana Olga Zhigalinabc Svetlana Sizovad Vladimir Oleinikovd Dmitriy Khmeleninb Irina Dyachkovab Denis Zolotovb Alexey Buzmakovb Victor Asadchikovb Sergey Khaidukovd Ivan Kozlove
https://doi.org/10.1016/j.dental.2022.03.003 Dental Materials Available online 11 March 2022
Highlights
- •
-
Dynamic light scattering - new method for assessing the stability of the oxide layer of medical devices has been developed.
- •
-
The parameters of nanoparticles determine the surface quality of dental implants.
- •
-
Particle size, change in the signal intensity parameters with high reliability during statistical data processing.
- •
-
Elemental composition of supernatants agrees with the results of elemental analysis of dental implants themselves.
OBS: Most importantly, they proved that aluminum and other elements come off the implant.
OBS: Mais importante, eles provaram que o alumínio e outros elementos saem do implante.
Destaque para: "Deve-se notar que na área de implante estudada, há uma dispersão significativa de tamanhos de partículas, de dezenas de nanômetros a vários mícrons. Partículas grandes de tamanhos microns e submicrons contêm principalmente Ti, Al, O (Fig. 13, Fig. 15). São aparentemente pequenos fragmentos da camada superficial do implante e partículas de óxido de alumínio, que são detectados no corpo do implante pelo método SEM."

Abstract
Objectives
To study the oxide layer stability of certified dental implants of system "P", made based on TiO2 alloy with carbon coating. To perform a comparative statistical analysis of the obtained data with the available data for the dental implants of systems "A" and "B".
Methods
X-ray microtomography and X-ray fluorescence analysis were used to study soft tissue biopsy specimens. Supernatants were studied by dynamic light scattering and transmission electron microscopy when simulating free emission of nanoscale metal oxide particles from the surface of dental implants as well as when simulating physical loading. A comparative analysis of three parameters of nanoscale particles was performed by statistical data analysis. The surface of the "P" system dental implant with surface treatment was analyzed by scanning electron microscopy.
Results
Both free emission of nanoscale oxide layer particles and yield of nano- and microscale particles during simulation of physical load were confirmed. Statistically significant differences were noted in a comparative analysis of the size and frequency of occurrence of these particles in the supernatants obtained from the surfaces of three dental implant systems. The elemental composition of the particles and the composition and structure of the "P" system dental implants themselves were analyzed.
Significance
The developed method of dynamic light scattering can be used to compare the stability of the oxide layer of standardized medical products manufactured on the basis of the TiO2 alloy.
1. Introduction
Despite the wide variability of existing dental implant systems, most of which are made of titanium alloy, it should be noted that there are differences in surface treatment, internal and external thread characteristics, joint geometry with orthopedic constructions, and the shape of the medical devices themselves [1], [2]. The implant surface is the first structure in contact with the patient's blood, when inserting screw dental implants into the bone bed of the jaws. The treatment and quality of the medical device surface become the primary advantage of physiological processes over pathophysiological ones [3]. Osteointegration as a positive outcome of physiological reparation of the bone bed tissues, rather than fibroosteointegration with subsequent development of mucositis and periimplantitis, leading to loss-disintegration of dental implants, is considered today from the position of possible particle emission [4]. There is currently no standardized way to assess the stability of the oxide layer of medical devices over time, in particular dental implants, using nanotechnology approaches. In addition, it is impossible to perform a comparative analysis of the quality and stability of alloys and their surface treatment in certified medical devices by technology and composition not disclosed by manufacturers at the level of free emission of nanoscale particles, and the yield of particles during simulation of physical loading involved in the process of both osseointegration and disintegration of dental implants.
It is assumed by the authors that nanoscale metal particles (NSMP) located in the oxide layer of dental implants can be participants in both the process of osseointegration and disintegration of dental implants when they critically accumulate in tissues and form complexes of nanoscale particles in the form of microparticles.
The analysis of modern literature has revealed a tendency to study the topography of the dental implant surface itself [5], [6], their composition in terms of the elemental ratio in the product alloy and the oxide film [7], as well as the surface treatment of dental implants by various methods with the coating of different structures [8], [9], [10], [11], [12].
When studying the methods of prevention or therapy of mucositis and peri-implantitis, the treatment of implant surfaces by applying nanoparticles with antibacterial activity is relevant. In [13], [14], [15] the authors note that the negative aspect of such coating is the result of particles emission from the dental implants surface and their accumulation in tissues as a toxic effect for the emergence of an inflammatory reaction of the body.
Earlier studies by methods of dynamic light scattering and electron microscopy of the formation and free emission of NSMP from the surface of metal medical products allowed to assess the surface quality of dental implants of systems from various manufacturers [16], [17], [18]. In this work by methods of dynamic light scattering and transmission electron microscopy the supernatants have been investigated during simulation of free emission of nanoscale metal particles of the oxide layer from the surface of 60 units of dental implants undergoing carbon surface treatment as well as during simulation of physical loading. These studies will make it possible to obtain and analyze the stability of the oxide layer of medical products under laboratory conditions using dental implants of three manufacturers' systems with different surface treatments, simulating immersion into the bone bed and mechanical loading.
2. Materials and methods
2.1. Clinical case
2.1.1. Patient G., (female), 55 years old
At the Department of Oral Surgery No. 2 of Moscow State University of Medicine and Dentistry, a dental implant surgery by system "A" was performed on patient G. with directed bone regeneration on both sides of the upper jaw using the patient's platelet-rich plasma Platelet-Rich Fibrin (PRF). Platelet-Rich Fibrin was used as a membrane, as well as bone-plastic material "BioOss", six months after teeth 14, 15, 24, 25 were extracted. During the second surgical stage of dental implantation, after another six months, fibrous capsules above the dental implants' surface were detected, and bone resorption in the cervical area of the dental implants to a depth of 3 mm. The fibrous capsules were removed and studied by X-ray microtomography and X-ray fluorescence analysis. The bone defects were closed with connective tissue grafts taken from the mucosa of the alveolar process of the hard palate.
The presented clinical case served as the basis for the studies conducted in this work. Namely, the laboratory study of both the structure of the implants themselves and the composition of the oxide layer, patented by the manufacturer, in terms of the stability of the coating when physically used as a support, prior to their clinical use.
2.2. X-ray microtomography
A soft tissue biopsy (fibrous capsule) obtained from the oral cavity of a patient with clinical signs of a chronic inflammatory process (see 2.1) was studied by X-ray microtomography to identify and visualize particles involved in the process of both osseointegration and disintegration of dental implants. Tomographic measurements of the sample were performed on a "TOMAS" laboratory microtomography setup [19]. A conventional X-ray tube with a molybdenum anode (17.5 keV energy) was used as the radiation source. The accelerating voltage and current values were 40 kV and 40 mA, respectively. The measurements were performed using a pyrolytic graphite monochromator crystal. The distance from the monochromator to the sample was 1.2 m, and the distance from the sample to the detector was 0.02 m. The size of the beam on the object was about 2 cm. In each experiment, 400 projections were taken in the angular range of 0–200°, in 0.5° increments and 5 s per frame exposure. A XIMEA-xiRay11 high-resolution X-ray detector was used in the measurements, which allows obtaining images with 9 µm spatial resolution and at a field of view of 36 × 24 mm. Reconstruction was performed with the algebraic method, followed by the procedure of processing the obtained 3D images.
2.3. X-ray fluorescence analysis (XRF)
The method of X-ray fluorescence analysis was used to obtain qualitative information on the elemental composition of a soft tissue biopsy sample (fibrous capsule) (see 2.1). Investigations were carried out on a "DITOM-M" diffractometer [20] with the X-123SDD detector-spectrometer (Amptek, USA). The radiation source was an X-ray tube with a molybdenum anode using a high-performance silicon crystal (111) as a monochromator. The spot size on the sample was ~4 mm vertically and ~1 mm horizontally. The range of obtained fluorescence spectra was from 1 to 17.479 keV (Kα1 molybdenum line) with an energy resolution of ~150 eV. The acquisition time of the spectra was 600 s.
2.4. Dynamic Light Scattering
In this work, 60 dental implants of the "P" system, 5.0–10.0 mm in size, that underwent carbon surface treatment were studied by dynamic light scattering. The method of dynamic light scattering (photon-correlation or quasi-elastic light scattering) is used to measure objects from 1 to 1000 nm in size, which makes it possible to record the output of the NSMP from the research objects.
The samples in study were subjected to vacuum-plasma sterilization. To prepare the supernatants, each dental implant of 60 units was placed in a test tube with 2 ml of bidi distilled water. In addition, 2 test tubes were prepared with bidiistilled water as a control. The samples were incubated for five days in a CO2 incubator at 37.2 ⁰C. This method was first developed to perform the basophilic test and is described in patent no. 2611013C1 [21].
Subsequently, the supernatants containing dental implants were subjected to ultrasound exposure at a frequency of 35 kHz with different time intervals, which was an in vitro simulation of the conditions of physiological immersion of dental implants into bone tissue and reproduction of physical load in laboratory conditions. As a result of the performed in vitro experimental studies supernatants with 60 units of "P" system dental implants were obtained under the conditions of free particle emission, as well as under the influence of 35 kHz ultrasound frequency for 0, 5, 15, and 35 min, respectively. Two test tubes with distilled water were used as the controls for studying each system in three experiments. The dynamic light scattering method was used to record measurements of three parameters: NSMP diameter (D, nm), frequency of NSMP occurrence in the supernatants (ACR, kcps), a polydispersity of NSMP in the supernatants (PD, %). In order to detect nanoparticles in the obtained supernatants and determine their size, studies were performed on a 90 Plus Particle Size Analyzer (Brookhaven Instruments Corporation, USA) in multimodal mode using the automatic 90Plus/BI-MAS function as well as the "dust cut-off" function that allows removing massive objects, particularly dust, from the counted nanoparticles. At the same time, the filter value was 20.
Statistical processing of the data obtained by dynamic light scattering on the "P" system dental implants was performed in comparison with the previously published results for the "A" and "B" systems [18].
2.5. Statistical studies
Statistical processing of the obtained results in the experiments on free emission of particles and estimation of reliability of changes performed using the Mann-Whitney U-test [22]. For statistical calculations of not normally distributed data, the Kolmogorov-Smirnov t-criterion [23] was used. Also, the Tukey criterion [24] was used to calculate the reliability of the data between the study subgroups:**−p<0.01***−p<0.001****−p<0.0001.
2.6. Electron microscopy
Observation of metallographic microstructures or defects by scanning electron microscopy (SEM) requires special sample preparation. To study the quality of the "P" system dental implant coating and visualize their structure under the coating, we obtained cross-sections slices that were prepared in several stages: implant pouring with resin, cutting, mechanical grinding, ion polishing. The implant was cut using a Leica EM TXP universal precision cutting system. The integrated stereomicroscope with a scale grid and adjustment of the sample holder angle to 60° (relative to the cutter rotation axis) provided complete visual control of the cutting process and mechanical grinding of the sample surface. Mechanical grinding was performed using grinding disks with successive reduction of the abrasive particle size from 15 to 0.5 µm (15–9–2–0.5 µm).
However, as it is known, traditional mechanical preparation of the sample can lead to the appearance of additional damages, defects that distort the actual structure of the coating. To avoid such artifacts and improve contrast in SEM images at the last stage, the method of ion etching was used in Hitachi IM4000plus, which allows for etching the sample surface with a wide beam of Ar+ ions with an energy up to 6 kV, quickly eliminates cutting defects, provides obtaining accurate cross-sections of large area (up to 5 mm2) without applying mechanical stress to the sample.
Obtaining a high-quality large-area sample surface for SEM studies is ensured in the following way. Since the ion beam has a Gaussian current density profile, when the center of the ion beam falling on the surface coincides with the rotation center of the sample, the central region of the sample material is etched at a higher rate than the neighboring areas of its surface. In the Hitachi IM4000plus unit, the positions of rotation and swing centers of the sample change relative to the center of the ion beam; hence a large area with increased homogeneity is treated in the etching process. Fig. 1 shows an SEM image of the implant cross-section: on the right - the area, treated by ion etching (smooth defect-free edge), on the left - only mechanical grinding (defects are visible).

Fig. 1. SEM image of the implant cross-section.
The structure of the implant surface was studied by scanning electron microscopy (SEM), transmission electron microscopy (TEM), scanning transmission electron microscopy (STEM) with z-contrast, electron diffraction, and energy-dispersive analysis (ED) using a Scios scanning electron microscope (secondary electron mode, Everhardt-Thornley detector) at accelerating voltages from 2 to 20 kV and an FEI Tecnai Osiris transmission electron microscope with field emission at an accelerating voltage of 200 kV. The FEI Tecnai Osiris SuperX EDS system allows rapidly obtaining (for several minutes) large area maps of chemical element distribution. Electron microscopy images were processed and analyzed using the Digital Micrograph, Esprit, TIA, and JEMS software. For TEM studies, supernatants prepared uniquely [17] with nanosized particles obtained from the surface of the "P" system dental implants were applied to copper grids with a thin substrate of amorphous carbon.
3. Results and discussion
Fig. 2 shows the results of tomographic studies of a soft tissue biopsy sample from the oral cavity in the area of previously installed dental implants of the "А" system.
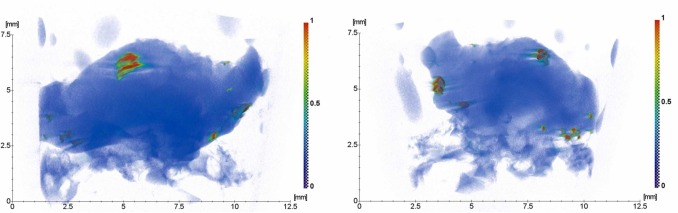
Fig 2. Results of three-dimensional reconstruction of soft tissue biopsy specimens.
Extraneous strongly absorbing microinclusions with sizes from tens of microns to several millimeters were detected (Fig. 2, contrast by absorption coefficient from green to red). From the analysis of the absorption coefficient, it can be assumed that larger inclusions are, apparently, hydroxyapatite. To identify small inclusions with a higher absorption coefficient, samples of soft tissue biopsy specimens were studied using XRF. The analysis of the XRF studies showed that the following elements were present in the biopsy specimen (Fig. 3): Si, P, S, Ca, Ti, Co, Ni, Zn, Sr, Br.
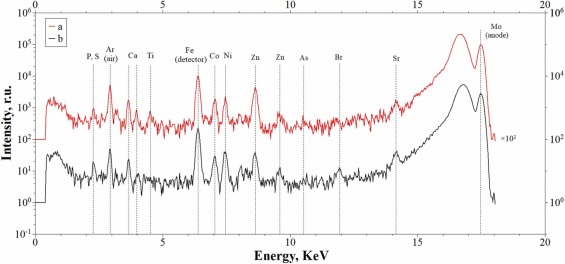
Fig 3. The X-ray fluorescence spectrum of the biopsy sample in study: (a) - 1 mm from the edge; (b) - 2.5 mm from the edge.
The study of supernatants containing nanoscale particles from the surfaces of "P" system dental implants after incubation in a CO2 incubator and free emission of particles, as well as after treatment by ultrasound with simulated physical load under in vitro conditions and different exposure time range showed the yield of nanoscale particles from the surface of all the samples studied (N) (Fig. 4).
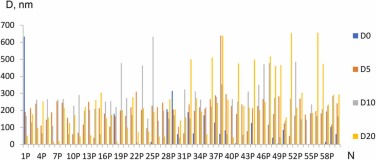
Fig 4. Particle sizes in the supernatants after incubation of implants of the "P" system in distilled water for five days without mechanical and physical action - free particle emission (0 min, the first particle pool, D0) and after treatment with ultrasound at a frequency of 35 kHz for 5 (D5), 15 (D10), 35 (D20) minutes.
As can be seen from the results presented in Fig. 5, in almost all cases, the ACR value (frequency of occurrence of objects) increases with increasing ultrasonic exposure time, i.e., the total number of particles increases during ultrasonic treatment.
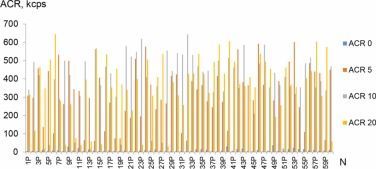
Fig 5. Change of ACR signal intensity - frequency of occurrence of NSMP in the supernatants obtained from the surfaces of dental implants of the "P" system, with free emission of NSMP (ACR0) and depending on the time of ultrasound treatment: 5 (ACR5), 15 (ACR10), 35 (ACR20) minutes.
At the same time, treatment of supernatants with ultrasound decreases the polydispersity coefficient (Fig. 6.), indicating that the available particle aggregates tend to disintegrate under such exposure.
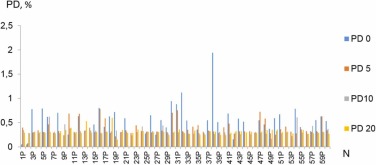
Fig 6. Changes in the value of polydispersity coefficient PD of NSMP in the supernatants obtained from the surfaces of dental implants of the "P" system, with free emission of NSMP (PD0) and depending on the time of ultrasound treatment: 5 (PD5), 15 (PD10), 35 (PD20) minutes.
For performing a comparative analysis of the three dental implant systems, a conclusion can be made about the nature of NSMP emission, both when simulating physiological embedding and when simulating physical loading under in vitro conditions. Fig. 7 shows the results of statistical processing of data on the three studied parameters: D (nm), ACR (kcps) and PD (%) of the dental implant system "P", as well as in comparison with two other implant systems: "A" and "B" (Fig. 8, Fig. 9).
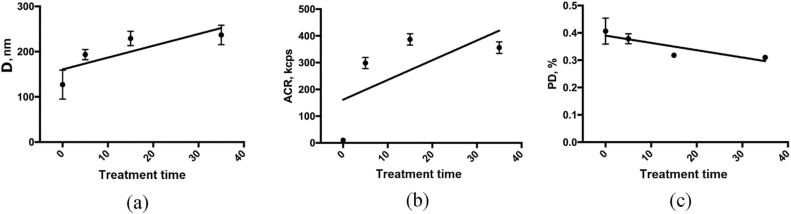
Fig 7. Changes in diameter (a), frequency of occurrence (b), and polydispersity (c) of NSMP in supernatants when exposed to ultrasound for 0, 5, 15, 35 min at a frequency of 35 kHz in the "P" system.
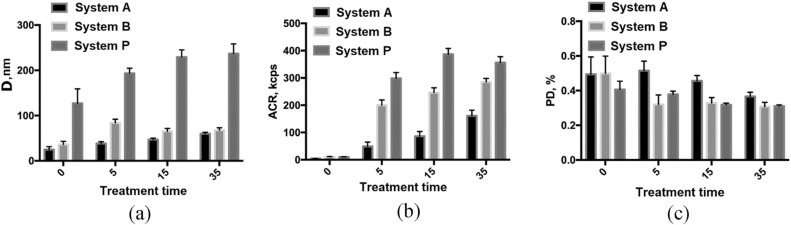
Fig 8. Comparative analysis of changes in diameter (a), frequency of occurrence (b), polydispersity (c) of NSMP in supernatant compositions when exposed to ultrasound for 0, 5, 15, 35 min at 35 kHz in the "A", "B", and "P" systems.
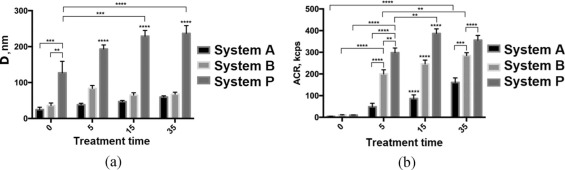
Fig 9. Statistical analysis of changes in diameter (a) and frequency of occurrence (b) of NSMP in supernatant compositions when exposed to ultrasound for 0, 5, 15, 35 min at 35 kHz in systems "A", "B", and "P".
From the presented results of statistical processing of the data, it can be concluded the following:
1. Significant differences were revealed according to the parameter of NSMP diameter in the supernatants, obtained from the dental implant surfaces of the "P" system at free emission and under the influence of ultrasound for 5, 15, 35 min between P0 and P15, ***p < 0.0003 and between P0 and P35, ****p < 0.0001 respectively.
2. Significant differences were revealed according to the parameter of NSMP frequency of occurrence in the supernatants, obtained from the surfaces of the "P" system dental implants at free emission and under the influence of ultrasound for 5, 15, 35 min respectively between P0 and P5, P15, P35, ****p < 0.0001, between P5 and P15, **p < 0.003 and between P5 and P35, ****p < 0.0001.
3. When comparing the results of polydispersity parameters for the three dental implant systems "A", "B", and "P", no reliable differences were found.
4. At comparative processing of statistical data, the reliable differences in the yield of NSMP, obtained from the surface of dental implants of the "P" system in comparison with the yield of NSMP, obtained from the surfaces of dental implants of the "A" system by the parameter of particle diameter at different time intervals are from p < 0.014 to p < 0.0001.
5. At comparative processing of statistical data, the reliable differences in the yield of NSMP, obtained from the surface of dental implants of the "P" system in comparison with the yield of NSMP, obtained from the surfaces of dental implants of the "B" system by the parameter of particle diameter in different time intervals are from p < 0.0061 to p < 0.0001.
6. At comparative processing of statistical data, the reliable differences in the yield of NSMP, obtained from the surface of dental implants of the "P" system in comparison with the yield of NSMP, obtained from the surfaces of dental implants of the "A" system by the parameter of frequency of occurrence in different time intervals are p < 0.0001.
7. At comparative processing of statistical data, the reliable differences in the yield of NSMP, obtained from the surface of dental implants of the "P" system in comparison with the yield of NSMP, obtained from the surfaces of dental implants of the "B" system by the parameter of frequency of occurrence in different time intervals are from p < 0.0045 to p < 0.0001.
The composition and structure of the "P" system dental implant surface, that underwent carbon surface treatment were also studied by SEM and PEM methods in this work. Fig. 10 a, b, c show SEM images of the implant surface, where non-uniform contrast - dark and light areas are observed. Such contrast in the SEM secondary electrons mode can be associated not only with the peculiarities of electron scattering, but also with disturbances in the continuity or chemical composition of the coating. It is necessary to note the developed relief on the sample surface, which is clearly visible at high magnifications (Fig. 10 c). In order to find out what caused the different contrast, the chemical composition of the implant surface was examined in the scanning electron microscope by the method of energy dispersive analysis.

Fig 10. SEM images of the implant surface: (a) general view; (b) enlarged area, with the numbers 1–3 indicating the points where the quantitative ED analysis was performed; (c) surface topography.
Fig 10 b shows the implant surface area and points (1, 2, 3), where spectra were obtained, and quantitative elemental analysis was performed by Kα line. The results of this analysis are presented in Table 1.
Table 1. Composition of surface layers (at%) at points 1, 2, 3, shown in Fig. 10 b.
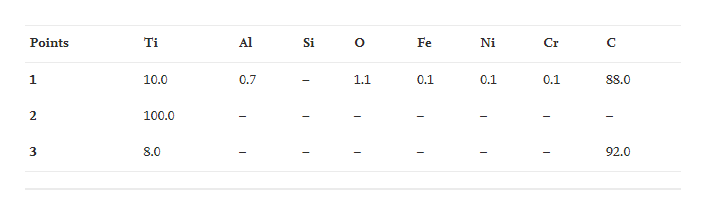
As can be seen from a comparison of the results, the elemental composition varies somewhat from one point to another. The main elements are C and Ti (points 1 and 3), but in some areas, possibly in the areas of coating damage, Al, Fe, Cr, and Ni may be present in small amounts.
SEM study of specially prepared cross-sections (as described above in section 2.6, Fig. 1) gives more detailed information about the quality and continuity of the coating. Fig. 11 shows SEM images of the coating areas on the implant surface and adjacent areas.

Fig 11. SEM images of the implant cross-section edge: (a) coating area without defects; (b-d) cracks, defects, and inclusions in the surface layer.
Different areas can be seen on the edge of the implant: with a continuous coating (Fig. 11 a), with cracks and discontinuities (Fig. 11 b, d), with no coating in some areas (Fig. 11 d), and with inclusions up to several microns in size (Fig. 11 b, c, d). The inclusions can be in the implant body or protrude to the surface, disrupting the continuity of the coating and leading to cracking (Fig. 12 a). Microcracks are also present in some inclusions' bodies. The ED analysis revealed the difference in the chemical composition of the surface and subsurface layers, i.e., in the implant body where N and C are present (Table 2, Fig. 12 b). Chemical analysis of the inclusions, performed by obtaining chemical elemental distribution mapping, showed that the inclusions are aluminum oxides (Fig. 12 c).

Fig 12. SEM image of an aluminum oxide inclusion (a) and elemental distribution mapping of the implant body area (b), the inclusion (c).
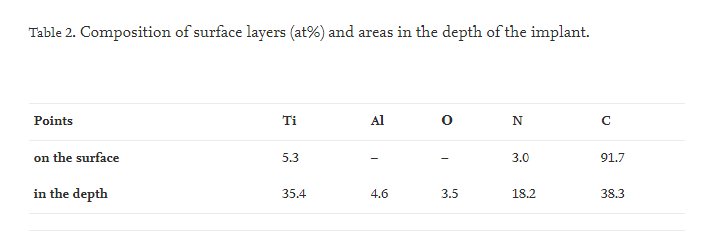

Fig. 13, Fig. 14, Fig. 15, Fig. 16 shows the results of TEM studies of metal-containing particles found in the tissues surrounding the implant surface: STEM images with z-contrast, chemical element distribution mapping, and corresponding ED spectrums.
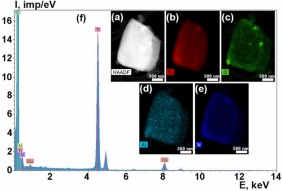
Fig 13. STEM image of the particle with z-contrast (a); chemical element distribution maps (b-e): ED spectrum (f).
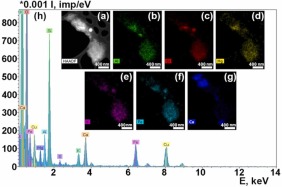
Fig. 14. STEM image of the particle with z-contrast (a); chemical element distribution maps (b-g): ED spectrum (h).
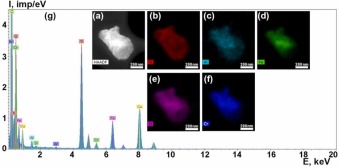
Fig. 15. STEM image of the particle with z-contrast (a); chemical element distribution maps (b-f): ED spectrum (g).
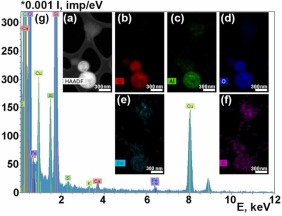
Fig. 16. STEM image of the particle with z-contrast (a); chemical element distribution maps (b-f): ED spectrum (g).
It should be noted that in the studied implant area, there is a significant scattering of particle sizes, from tens of nanometers to several microns. Large particles of micron and submicron sizes contain mainly Ti, Al, O (Fig. 13, Fig. 15). They are apparently small fragments of the implant surface layer and aluminum oxide particles, which are detected in the implant body by the SEM method. The chemical elements most frequently present in the particle spectra are Ti, Al, O, Fe, N, Si, P, K, Ca. Cr, S, and Mg also occur in small amounts (Fig. 14, Fig. 15, Fig. 16). The Cu peaks for all spectra obtained in the transmission electron microscope appear due to a copper grid on which the particles under study were deposited. Since the particles were on a carbon substrate, it is impossible to judge the content of C in their composition.
4. Conclusion
According to the results of the studies, it can be concluded that the detected NPMFs have emission properties both in the process of successful osseointegration of dental implants and are participants in the early complications related to bone resorption. In the presented clinical case, X-ray microtomography studies revealed the presence of large inclusions up to several millimeters in size within the fibrous capsules. Based on the absorption coefficient analysis, these inclusions appear to be hydroxyapatite. The presence of metal microelements in the fibrous capsule above the cervical area of a dental implant can only be a consequence of its introduction and mechanical loading on the osseointegrated implants. The obtained results of X-ray studies created prerequisites for the development of a method to assess the stability of the oxide layer of standardized medical products, in particular, dental implants during simulation of immersion into the bone bed and mechanical loading.
The elemental composition of the used alloy is known, and surface treatment of certified medical devices differs from manufacturer to manufacturer. Currently, there is no standardized method for assessing the stability of the oxide layer of dental implants at the level of nanoscale particles. For the first time, a laboratory method to identify the peculiarities of long-term use of dental implants as mechanical support were developed, taking into account the peculiarities of surface treatment. In this research and comparative analysis of the three dental implant systems it was found reliable differences in such parameters like the frequency of occurrence of NSMP (ACR, kcps) and particle size (D, nm). The smaller these parameters are, the more stable the dental implant surface is.
The structure of the "P" system dental implants surface, as well as the composition of surface and subsurface areas, were studied by electron microscopy and energy dispersive microanalysis methods. It was shown that on the surface, there is a 1–2 µm' thick layer, containing mainly Ti, C, and N. The coating reveals defects - cracks, discontinuities. Most of the coating defects are concentrated on non-planar parts of the surface - ribs. Inclusions of aluminum oxides of up to several microns in size are present both in-depth and on the surface of the implants. The elemental composition in the depth of implants differs from the surface layer composition by the presence of N and higher Al content.
The analysis of the supernatants revealed the presence of particles from a few microns to 40–50 nm in size, containing mainly such elements as Ti, Al, Si, O, N, and in smaller amounts Fe, Cr, Mg, K, P, Ca, S, which agrees with the results of elemental analysis of the implants themselves.
Based on the obtained results, it is essential to note that the coatings do not exclude the release of particles from the internal structure of the medical device itself and require compliance with the elemental composition according to ISO classification [25] in the manufacture of medical products from materials based on TiO2.
